|
European Medicines Agency - - Praluent. This is a summary of the European public assessment report (EPAR) for Praluent. It explains how the Agency assessed the medicine to recommend its authorisation in the EU and its conditions of use. It is not intended to provide practical advice on how to use Praluent. For practical information about using Praluent, patients should read the package leaflet or contact their doctor or pharmacist. What is Praluent and what is it used for? Praluent is a medicine used to treat adults with primary hypercholesterolaemia (high blood cholesterol levels, in particular of the type . Primary means that the disease is generally the result of a genetic abnormality. Primary hypercholesterolaemia includes heterozygous familial (when the genetic abnormality is inherited from only one parent) and non- familial disease (when the genetic abnormality arises spontaneously without a family history). Praluent is also used to treat mixed dyslipidaemia (abnormal levels of fats in blood, including high levels of LDL- cholesterol). Praluent is to be used together with a low- fat diet, in the following ways: in combination with a statin (other cholesterol- lowering medicines), or a statin plus other fat- lowering medicines, in patients who do not adequately respond to the maximum tolerated dose of the statin; alone or in combination with other fat- lowering medicines in patients who cannot tolerate or cannot be given statins. Praluent contains the active substance alirocumab. 
How is Praluent used? Before starting treatment with Praluent, other causes of excess cholesterol and abnormal fat levels in the blood should be excluded. The medicine can only be obtained with a prescription. 
Praluent is available as a solution for injection in a pre- filled syringe or pre- filled pen (7. The injection is given under the skin of the abdomen, thigh or upper arm. The usual starting dose is 7. The dose of Praluent is adjusted based on the levels of fats in blood and response to the medicine. If the desired response is not achieved after 4 weeks of treatment, the doctor can increase or decrease the dose. Patients or their carers can inject the medicine once they have been properly trained by a healthcare professional. For more information, see the package leaflet. How does Praluent work? The active substance in Praluent, alirocumab, is a monoclonal antibody. A monoclonal antibody is an antibody (a type of protein) that has been designed to recognise and attach to a specific structure (called an antigen) in the body. Alirocumab has been designed to attach to a protein called . This protein attaches to cholesterol receptors on the surface of liver cells and causes these receptors to be absorbed and broken down inside the cells. These receptors control blood levels of cholesterol, especially LDL- cholesterol, by removing it from the bloodstream. 
By attaching and blocking PCSK9, Praluent prevents the receptors from being broken down inside cells and therefore increases the number of these receptors on the cell surface, where they can attach to LDL- cholesterol and remove it from the bloodstream. This helps to reduce the amount of cholesterol in the blood. What benefits of Praluent have been shown in studies? Praluent has been studied in 1. Some studies looked at Praluent taken on its own, while others studied Praluent in combination with other fat- lowering medicines, including patients on the maximum recommended doses of statins. Some studies compared Praluent with placebo (a dummy treatment) and others to another medicine for hypercholesterolaemia (ezetimibe). ARUP Laboratories is a national reference laboratory and a worldwide leader in innovative laboratory research and development. ARUP offers an extensive lab testing. This is a summary of the European public assessment report (EPAR) for Praluent. It explains how the Agency assessed the medicine to recommend its authorisation in the. 
With 80,000 users in 8 years, my invention Gastric Bypass ALTERNATIVE (NO Surgery) helped users achieve a healthy weight WITHOUT risky bariatric surgery. COLABORACIÓN ESPECIAL. Nutrición y síndrome metabólico. Nutrition and Metabolic Syndrome. Pilar Matía Martín, Edurne Lecumberri Pascual y Alfonso L. 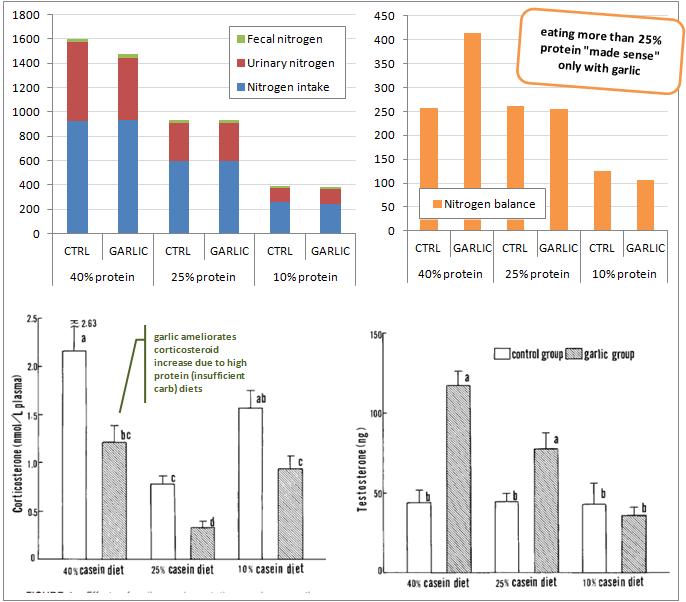
These studies showed that when Praluent was given on top of a statin it led to a substantial reduction in blood levels of LDL- cholesterol (between 3. When given on top of standard treatment or on top of placebo, Praluent produced a 2. LDL- cholesterol than ezetimibe. What are the risks associated with Praluent? The most common side effects with Praluent (which may affect up to 1 in 1. 
For the full list of side effects and restrictions, see the package leaflet. Why is Praluent approved? The Agency’s Committee for Medicinal Products for Human Use (CHMP) decided that Praluent’s benefits are greater than its risks and recommended that it be approved for use in the EU. 2 This medicinal product is subject to additional monitoring. This will allow quick identification of new safety information. Healthcare professionals are asked to. The test menu below is a complete list of ARUP’s inherited disease testing. A patient history form is requested for many of these genetic tests. The Committee noted that across all studies in patients with primary hypercholesterolaemia and mixed dyslipidaemia, including patients on maximum recommended doses of statins or those intolerant to them, Praluent showed an important reduction in LDL- cholesterol levels, which is a known risk factor for cardiovascular (affecting the heart and blood vessels) disease. It is not yet known, however, whether Praluent will reduce cardiovascular disease, as data on long- term cardiovascular outcomes are still pending. Therefore, Praluent has been approved for use in patients who do not adequately respond to the maximum tolerated dose of statins or who cannot be given statins. With regard to safety, the Committee noted an acceptable safety profile. 
What measures are being taken to ensure the safe and effective use of Praluent? A risk management plan has been developed to ensure that Praluent is used as safely as possible. Based on this plan, safety information has been included in the summary of product characteristics and the package leaflet for Praluent, including the appropriate precautions to be followed by healthcare professionals and patients. Further information can be found in the summary of the risk management plan. Other information about Praluent. The European Commission granted a marketing authorisation valid throughout the European Union for Praluent on 2. September 2. 01. 5. For more information about treatment with Praluent, read the package leaflet (also part of the EPAR) or contact your doctor or pharmacist. This EPAR was last updated on. Early Signs, Symptoms & Treatment. Parkinson's Disease Diet and Nutrition. Maintaining Your Weight With Parkinson's Disease. Malnutrition and weight maintenance is often an issue for people with Parkinson's disease. Here are some tips to help you maintain a healthy weight. Weigh yourself once or twice a week, unless your doctor recommends weighing yourself often. If you are taking diuretics or steroids, such as prednisone, you should weigh yourself daily. If you have an unexplained weight gain or loss (2 pounds in one day or 5 pounds in one week), contact your doctor. He or she may want to modify your food or fluid intake to help manage your condition. Avoid low- fat or low- calorie products. Use whole milk, whole milk cheese, and yogurt. Parkinson's disease facts. Parkinson's disease is a neurodegenerative disorder which leads to progressive deterioration of motor function due to loss of dopamine- producing brain cells. Primary symptoms includetremor,stiffness,slowness,impaired balance,and later on a shuffling gait. Some secondary symptoms include. Most individuals with Parkinson's disease are diagnosed when they are 6. Parkinson's disease also occurs. With proper treatment, most individuals with Parkinson's disease can lead long, productive lives for many years after diagnosis. What is Parkinson's disease? Parkinson's disease is the second most common neurodegenerative disorder and the most common movement disorder. It is characterized by progressive loss of muscle control, which leads to trembling of the limbs and head while at rest, stiffness, slowness, and impaired balance. As symptoms worsen, it may become difficult to walk, talk, and complete simple tasks. The progression of Parkinson's disease and the degree of impairment vary from individual to individual. Many people with Parkinson's disease live long productive lives, whereas others become disabled much more quickly. Premature death is usually due to complications such as falling- related injuries or pneumonia. Most individuals who develop Parkinson's disease are 6. Since overall life expectancy is rising, the number of individuals with Parkinson's disease will increase in the future. Adult- onset Parkinson's disease is most common, but early- onset Parkinson's disease (onset between 2. Parkinson's disease (onset before age 2. Descriptions of Parkinson's disease date back as far as 5. BC. Around that time, an ancient Indian civilization called the disorder Kampavata and treated it with the seeds of a plant containing therapeutic levels of what is today known as levodopa. Parkinson's disease was named after the British doctor James Parkinson, who in 1. Most of the movement- related symptoms of Parkinson's disease are caused by a lack of dopamine due to the loss of dopamine- producing cells in the substantia nigra. When the amount of dopamine is too low, communication between the substantia nigra and corpus striatum becomes ineffective, and movement becomes impaired; the greater the loss of dopamine, the worse the movement- related symptoms. Other cells in the brain also degenerate to some degree and may contribute to non- movement related symptoms of Parkinson's disease. Although it is well known that lack of dopamine causes the motor symptoms of Parkinson's disease, it is not clear why the dopamine- producing brain cells deteriorate. Genetic and pathological studies have revealed that various dysfunctional cellular processes, inflammation, and stress can all contribute to cell damage. In addition, abnormal clumps called Lewy bodies, which contain the protein alpha- synuclein, are found in many brain cells of individuals with Parkinson's disease. The function of these clumps in regards to Parkinson's disease is not understood. In general, scientists suspect that dopamine loss is due to a combination of genetic and environmental factors. What genes are linked to Parkinson's disease? In most individuals, Parkinson's disease is idiopathic, which means that it arises sporadically with no known cause. However, some of individuals diagnosed with Parkinsons also have family members with the disease. By studying families with hereditary Parkinson's disease, scientists have identified several genes that are associated with the disorder. Studying these genes helps understand the cause of Parkinson's disease and may lead to new therapies. So far, five genes have been identified that are definitively associated with Parkinson's disease. SNCA (synuclein, alpha non A4 component of amyloid precursor): SNCA makes the protein alpha- synuclein. In brain cells of individuals with Parkinson's disease, this protein aggregates in clumps called Lewy bodies. Mutations in the SNCA gene are found in early- onset Parkinson's disease. PARK2 (Parkinson's disease autosomal recessive, juvenile 2): The PARK2 gene makes the protein parkin. Mutations of the PARK2 gene are mostly found in individuals with juvenile Parkinson's disease. Parkin normally helps cells break down and recycle proteins. PARK7 (Parkinson's disease autosomal recessive, early onset 7): PARK7 mutations are found in early- onset Parkinson's disease. The PARK7 gene makes the DJ- 1 protein, which may protect cells from oxidative stress. PINK1 (PTEN- induced putative kinase 1): Mutations of this gene are found in early- onset Parkinson's disease. The exact function of the protein made by PINK1 is not known, but it may protect structures within the cell called mitochondria from stress. LRRK2 (leucine- rich repeat kinase 2): LRRK2 makes the protein dardarin. Mutations in the LRRK2 gene have been linked to late- onset Parkinson's disease. Several other chromosome regions and the genes GBA (glucosidase beta acid), SNCAIP (synuclein alpha interacting protein), and UCHL1 (ubiquitin carboxyl- terminal esterase L1) may also be linked to Parkinson's disease. Who is at risk for Parkinson's disease? Age is the largest risk factor for the development and progression of Parkinson's disease. Most people who develop Parkinson's disease are older than 6. A small number of individuals are at increased risk because of a family history of the disorder. Medically Reviewed by a Doctor on 8/9/2.
0 Comments
Leave a Reply. |
AuthorWrite something about yourself. No need to be fancy, just an overview. Archives
August 2017
Categories |
 RSS Feed
RSS Feed
